No matter where I am or what I am doing – support groups, workshops, or training – the same question always comes up. What is the difference between Alzheimer’s and Dementia? I sometimes want to ask, “Why? Does it really matter to a caregiver?”
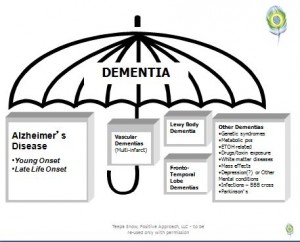
“Dementia” refers to a group of symptoms brought on by diseases, trauma, or illnesses that affect the brain. These symptoms include loss of memory, motor skills, and cognitive brain function. There are nearly 100 different causes for dementias. Alzheimer’s is a specific disease that is the most common cause of dementia. It is one cause that falls under the greater umbrella of dementia. To illustrate, I have used here a graphic developed by Teepa Snow for her Positive Approach to Care.
Alzheimer’s is a progressive and terminal disease, which means that a person will eventually die from complications from Alzheimer’s unless he or she dies from other causes. Medications are available, but they will only slow the progression of symptoms; not change the disease process or its prognosis. Alzheimer’s is the only disease among the top 10 causes of death in Americans that can’t be prevented, cured, reversed, or go into remission.
The number of Americans with Alzheimer’s disease and dementia is estimated to soar to 7.1 million by 2025; a 40 percent increase from the 5.1 million affected this year, according to the 2015 Alzheimer’s Disease Fact and Figures report published by the Alzheimer’s Association. The picture doesn’t improve for the foreseeable future since by 2050 it is projected that there will be 13.8 million sufferers.
On a side note, let me add here that you will hear people talk about reversible dementias. There are no reversible dementias. Sometime relative minor curable maladies can cause symptoms similar to dementia; but they are not true dementia.
Alzheimer’s disease is not a part of normal aging, and it is not restricted to the old. It is a disease that can afflict an individual in their 40s or 50s. According to the Alzheimer’s Association, life expectancy after symptoms become evident is eight to twelve years, but some can survive with Alzheimer’s as long as 20 years, depending on age and conditions.
As this disease progresses, it begins to have an effect on a person’s ability to conduct many of their daily activities. Many people still think it’s a disease that involves only the loss of memory. You do lose memory, but is so much more than that. Dementia goes beyond memory, executive functioning, and judgment. It also results in reduced vision, distorted hearing, and loss of motor skills. These degradation impact your ability to do every-day things, like getting dressed, walking, talking, bathing yourself, driving, and eating. Simple activities of daily living become a significant challenge. Memory loss is only one of the results of a disease that results in “Brain Failure.”
This is often denied by both the afflicted and their family members. They will grasp on anything that seems to validate that things are still “normal.” “My mom can’t have dementia, she can still play cards!” Reactions like this are common because it is hard to understand how someone who still demonstrates fairly complex thinking—like playing cards or crossword puzzles—can also show signs of dementia.
In these cases, very familiar routines and environments—like playing cards in one’s home—make it easier for the person to continue to appear normal, for the most part. Performing rote activities may help cover up deficits in thinking. On the other hand, less familiar environments and activities, like navigating through an airport, changing the game of cards, dining in a different restaurant, can make the signs of dementia much more obvious. You may see frustration, anger, repetition in conversation, and other behaviors that indicate they are uncomfortable or may not be able to cope with the situation. Their behaviors are always telling you something, and as a caregiver it is your task to try to figure it out. They are not just being difficult; they are calling for you to help them.
Each behavior by itself may not necessarily indicate dementia, but the presence of several of the classic behaviors can indicate dementia. It is also important to consider whether a particular behavior is a sign of change for the person. For example, if your loved one has always had trouble remembering dates, then forgetting dates may not be a significant warning sign. But if becoming angry, getting lost, or otherwise behaving differently from how they have in the past may indicate it is time to seek consultation with your physician.
If you do suspect that your loved one may have signs of early stages of dementia, it’s important to seek a diagnosis right away. Sometimes people want to avoid this knowledge, but refusing early diagnosis only takes away valuable time toward maximizing quality of life, benefiting from treatment, or simply allowing the victim to be a part of the very important planning that can benefit themselves and their caregiver as the disease progresses.
Testing can rule out, strokes, blood clots, thyroid, B levels, dehydration, urinary tract infection and other reparable problems that may falsely suggest dementia. Early diagnosis can also allow the caregiver to start networking, researching, and learning. You will need this as you move forward in this journey. As a caregiver, the one thing you will be able to count on is not if you will need help, but when you will decide to accept help. Trying to do it alone is a decision that you simply should not make. Help and experience is out there.
So knowing what the difference is between Alzheimer’s and dementia will not make much difference in understanding what you are up against. Knowing the medical fine points are not nearly as important as understanding how the disease will affect the caregiver. Rather, it is far more important to educate yourself on human factors of the disease; the behaviors and what causes them. Go to support groups; they are free and they are where you will glean much of the knowledge you will need. Stay social and keep your loved one social as long as you can.
Moreover, take care of yourself and realize this is not going to be a sprint; it is going to be a marathon. Having an understanding of what is happening will allow you to interact with your loved one in a calm, loving, compassionate, and caring way. Remember that it is not their fault and that they have no control over what is going on in their brain.
For the caregiver, it is a moot point whether it is Alzheimer’s, dementia, or whatever medical term may be applied to the condition. The important understanding is the knowledge and preparation for what is coming and how you can behave to make your and your loved one’s lives as peaceful and rewarding as possible during the process.
Until next time remember: “We all deserve the best”
Send your comments and stories to deb@coping.today
© Debbie Selsavage, 2015

It would be nice if the graphic could be expanded so we could actually read what it says. I can not read it at all.
Are you talking about the umbrella graphic? Here is the link to the graphic. Let me know if you need anything else.
https://www.google.com/imgres?imgurl=https://coping.today/wp-content/uploads/2015/08/Umbrella.jpg&imgrefurl=https://coping.today/what-is-the-difference-between-alzheimers-and-dementia/&h=368&w=457&tbnid=ipRAwPLC4OfZcM:&q=umbrella+of+dementia&tbnh=160&tbnw=199&usg=AI4_-kTLMwIjwClM_W8Fk0lDLjp8zRFA5w&vet=12ahUKEwit_IvTtdTdAhXMhSwKHRF1AdMQ9QEwAHoECAYQBg..i&docid=13AVoIXAMJ12jM&sa=X&ved=2ahUKEwit_IvTtdTdAhXMhSwKHRF1AdMQ9QEwAHoECAYQBg
Dementia is the symptoms and the actual disease of Alzheimer’s is under the umbrella, there are 120 types and forms od dementias under the umbrella. Alzheimer’s is just the most common one.
My brother thinks that medications would be different for treating a person with dementia compared to Alzheimer’s.
Hello Teresa,
There is no different drugs for dementia or Alzheimer’s they are using the same medications. There is only 5 medications they use, they will not do anything for the disease but you may see some leveling out with behaviors/moods. They have not had a drug for dementia or Alzheimer’s for more than 19 years these medications were used for other diseases. You can only treat the behaviors. Hope this helps.